VA Drives Innovation in Virtual Care for Patients and Clinicians
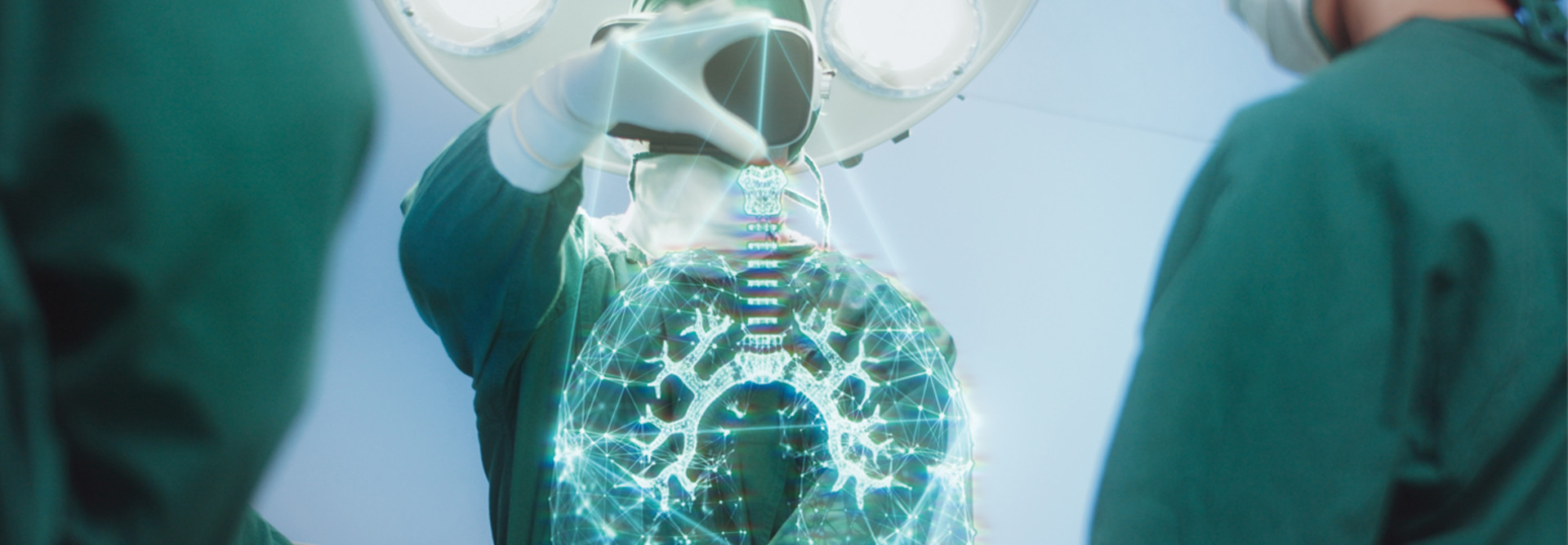
The VA has been working for more than a year on the Project Convergence initiative, which supports what the agency calls the “first-ever 5G-enabled augmented reality surgical navigation system,” helping it “deliver the most advanced surgical care available.”
Under Project Convergence, the VA has partnered with Verizon, medical AR technology company Medivis and Microsoft. The program brings Verizon’s 5G technology together with a Food and Drug Administration–approved use case for Medivis’ surgical AR clinical visualization software using Microsoft’s HoloLens 2 headset and Azure cloud service.
The VA has been focused on not just getting that technology out to clinical settings, but also thinking through the implications for its data and IT infrastructure, according to Vega.
There are several use cases the VA has flagged for VR and AR, Vegas says. One is rehabilitation, using VR headsets to conduct exposure therapy to treat post-traumatic stress disorder.
RELATED: How is the VA using 5G technology in hospitals?
A veteran, wearing a VR headset, can be guided through a traumatic experience virtually by a trained clinician. Such tools allow the VA to “recreate and explore” the experience and help acclimate veterans back into society, helping them to “feel whole again,” Vega says.
Another avenue is pain management. A veteran using VR can be distracted and guided to reimagine certain types of experiences. According to Vega, such therapy reduces the use of opiates for pain management as well as levels of pain, anxiety and depression.
“We’re seeing the promise,” Vega says. “For a lot of these, such as rehab, the veteran never leaves the home.” That can help connect and bring care to rural veterans especially.
MORE FROM FEDTECH: Find out how the Air Force is using virtual reality for training.
Vega notes that 70 percent of all doctors in the U.S. have received training in the VA healthcare system. “We have a mission to make sure we are exposing the future generation of doctors to the latest types of technology,” he said.
Other use cases include medical training, empathy training and pre-surgical planning. For example, doctors can use VR to practice intubation on a patient, and can perform simulations at home or away from a clinical setting. Training courses can also be democratized and made widely available, Vega noted.
Current technology enables the VA to project holographic images of a patient’s anatomy and layer it onto a patient, Vega says. He notes that 5G networks make this possible.
“We’re enabling things that we once believed to be science fiction,” Vega says. “Over the course of the next year, we’ll see more evolution.”
The use of AR and VR at those roughly 50 VA sites has come in the past 18 months and was accelerated by the coronavirus pandemic, Vega said. “If that type of spread and adoption can happen in 18 months, imagine what this looks like in 10 years.”
Follow FedTech coverage for more articles from Imagine Nation ELC 2021.